We’ve got some really sad news to share with you. Our beautiful, beloved Molly Dog…
Imposter Syndrome, Tall Poppies, Peer Leadership & Strategic Coproduction
In this blog I discuss strategic coproduction and peer leadership, the feeling of ‘imposter syndrome’ and the concept of ‘tall poppies’, and sharing my experiences of the above. I also share a definition of what I feel a peer leader is, and share some conversations had at the NHS England Personalised Care Strategic Coproduction Group yesterday. I discuss the importance of peer leaders like me sticking our head above the parapet, and encourage professionals to do the same. It was inspired by a blog by Kath Evans, entitled “Imposter Syndrome and Being A Tall Poppy”, which can be accessed here – https://kathevans.com/2019/05/15/dumping-imposter-syndrome-and-being-a-tall-poppy/. If you would like to find out more about the NHS England Strategic Coproduction Group, click here.
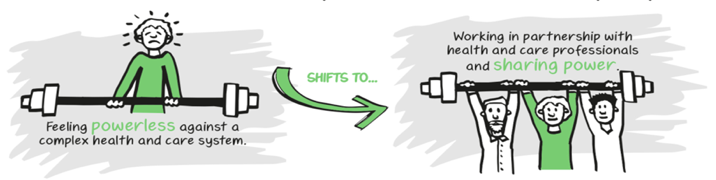
(c) NHS England
A friend of mine Kath Evans (Twitter: @KathEvans2) wrote on her blog this week about imposter syndrome and the concept of “tall poppies” that resonated deeply with me when I read it. You can read the blog here. She describes how she felt like an imposter when she first became a member of the Association for Chief Children’s Nurses (ACCN), wondering whether she was right to be part of it, that she could contribute and that she deserved to be there, and in her blog talks about ways to overcome that feeling of imposter syndrome. She also introduces a phrase and concept she’d heard of, “tall poppies” which Kath describes in the following quote from her blog:
“Many years ago I heard the phrase ‘tall poppies’ describing those people who stood out and had impact. Perhaps we need to consider how we become brave enough to stand tall, weather the challenges, always accept responsibility for our actions, learn, and move forward? I also wonder how we can support those who are growing to be tall poppies, our future generation of leaders, do we give them opportunities to shine? Perhaps we can all work to be more collaborative, inclusive, at making ourselves approachable and relatable? The leaders who role model these approaches, who encourage, open doors and nurture others I respect hugely.”
Kath comes at this blog in the healthcare professional/nurse context, but it resonated with me as applicable to peer/patient leaders and how we can feel when entering a new role, committee or project. We are sometimes the only non-professional in the room and even where we aren’t, when we first join we can struggle with this feeling of being an imposter and of not having a lot to contribute to that role and/or work. We may feel we do not have the comparable level of knowledge, skills and expertise. I sit on the NHS England Personalised Care Strategic Coproduction Group and we had our monthly meeting yesterday. At this meeting we discussed the fears of people who step into peer leadership-type roles, not knowing what to expect, feeling they couldn’t hold their own against expert professionals, feeling somewhat of an imposter who isn’t an expert, and a lot of peer leadership work is about empowering and supporting people to realise they have ‘personal power’, they bring the humanity and lived experience to the system and that their personal experience is bringing expertise of the system and how it works, whilst also recognising the need for peer leaders to understand the environment they’re working in, system structure, policies, frameworks and culture, and to be able to build effective working relationships with individuals and leaders within the system. So it can be quite overwhelming when you first start out as a peer leader, that feeling of insecurity and apprehension can lead to feelings of imposter syndrome. It’s important that people getting involved in the health system are treated and respected as experts, with a lot to contribute to the service, and that true strategic coproduction is utilised and done properly, all of theses are very important in supporting peer leaders to get started, build confidence and become a valued member of the health service in strategic coproduction and other activities.
What is a peer leader? At the Strategic Coproduction Group yesterday we discussed on our table the different terms and language and where they originate and how they are adopted and misused. A lot of people take issue at the term “patient leader”, denoting a sense of hierarchy between ‘ordinary’ patients and these patient leaders, but also carers and communities didn’t always identity with the word ‘patient’. Another individual at the SCG reminded us of the origin of the term ‘patient leader’ and how it was created by David Gilbert to redress the imbalance over the enforced term ‘patient’, transforming it from the passive recipient ethos of the term ‘patient’ to bringing it to seeing these individuals as leaders, people who have power and have a lot to bring and are experts in themselves, how they bring insider knowledge of the system and support and have the power to influence and effect change. Other terms we discussed were service user, patient and public voice member, expert by experience and others, and whether we like different terms – unanimously, our table disliked “service user” due to the denoting that you’re a “user” of services rather than an engaged expert. For me, I would describe a peer leader as follows: “A peer leader is a person who uses their lived experience to effect change within the system and who acts as a role model, who inspires, empowers and motivates people, brings them into the work but then leads and drives from behind, allowing and supporting people to realise their own potential, and who treats everyone as an expert and ensures there is no hierarchy.“. One young person shared her experience of sharing something on her social media produced by the NHS England Lived Experience team and the Strategic Coproduction Group and said how she was involved in its development, only to be told “no you can’t have been involved as that came from very high up in the NHS”. This is a damaging view of the personal power of peer leaders, our contributions to the health system, the knowledge and expertise we bring and the potential we have to influence, drive and effect change, be that nationally, regionally or locally. This lack of understanding of and respect for peer leaders can further perpetuate their feelings of being an imposter as they are not seen, valued or respected as ‘on the same level’ as the professionals in the room.
I certainly can attest to this imposter syndrome feeling and how the system often perpetuates this feeling amongst peer leaders. I got started in this work through my personal experience and wanting to make a difference, my hospice nurse nominating me to give my first speech, having previously done some filming for the hospice and been encouraged to start my blog. I went to that event, in a room full of MPs, Peers and eminent hospice, palliative care and health professionals, feeling somewhat like an imposter and almost quite inadequate. I gave a speech and made a huge impact, but that anxiety and apprehension about my role and how much I could bring to the table was ever-present. This was even more prominent when I began working with the health service directly and getting involved in committees, board and coproduction efforts. Even up to the last 2 years, turning up at a new committee or board and feeling like the imposter, feeling somewhat inadequate and feeling like I won’t be able to contribute effectively and ‘hold my own’ and be an effective voice for patients and elevating their experiences to the board. I felt especially like an imposter when I joined a NICE committee, as I joined later in the process due to being extremely ill when I was first selected to sit on the committee (Adult End Of Life Care Guideline Committee) in 2016 and feeling very much like I wasn’t as experienced and knowledgeable as the professionals on the committee, and perhaps didn’t have sufficient knowledge to aid me in that role. Other times I’ve felt like it was when I sat on the Children and Young People’s Health Outcomes Forum (which is where I first met Kath) before it was disbanded, and similarly when I first joined the NHS England Children with Complex Needs and SEND Board. Feeling like an imposter fosters a feeling of inadequacy and invalidation of your own power and experience. I am now a very confident and able peer leader, who works in many different ways with the NHS, healthcare, hospices, third sector and within research and even running networks for people interested in becoming peer leaders, for different projects, including the international palliative care patient and carer network, Palliative Care Voices. I have a deep understanding of the NHS, how the system works, the hierarchy and structure, the culture, policies, frameworks, funding and commissioning, how to build lasting working relationships with professionals and leaders within the system, to work with the system as it is with the realistic abilities within the system currently (in an ideal world a lot of things would happen and be different, but we don’t live in an ideal world) and how to affect change and use my power and expertise as a person with lived experience. It takes a lot of self-confidence, determination, persistence, a willingness to learn, the knowledge of the system and the ability to make connections and working partnerships with system leaders and professionals. However, I was recently elected to the new NHS Assembly and I can truly say I have rarely – outside the NHS England Strategic Coproduction Group – seen coproduction done so well, valuing peer leaders and their lived experience, involving us fully as partners and as people with power, and creating a level playing field where everyone is treated as an expert. I am excited to be on the Assembly and to be a peer leader bringing my own experience, as well as all the knowledge of the system, policies, culture, structure and so on and past experience working strategically and working and having positive relationships with system leaders.
Then there’s the concept of tall poppies and how this is interrelated with peer leadership. Peer leaders need to be prepared to stand tall, put their head above the parapet, weather the challenges they face in their role and maintain the energy and persistence despite these challenges and setbacks, and to take responsibility for our own role, actions and to be prepared to learn from others. Our role is also, crucially, about supporting others to become ‘tall poppies’ too, going back to the definition our table came up with at the Strategic Coproduction Group yesterday, we are role modelling, inspiring, motivating, empowering, leading by example and helping others to find their unique voice and realise their own potential. Being a tall poppy is sometimes challenging, it can be slow progress and seem like nothing is changing – change doesn’t happen quickly in a system like the NHS – and it can seem sometimes like our voices aren’t being heard, but advocating for proper strategic coproduction, leading by example, supporting the NHS to involve people with lived experience at all levels, in all aspects and in all sectors and departments of the NHS, from high-level strategy down to hands-on care, and to show them the benefit of involving peer leaders, this is our job, our duty and we can be ‘tall poppies’ and make a difference. Progress is progress, no matter how slow. We need to ensure patient and public voices are heard, lived experience is integral, and peer leaders are involved and our expertise and experience and our personal power are utilised. This is also about a shift in relationships, making patients equal partners, involving them in decisions not only in their own care but in the wider system and respecting and valuing patients as having power and expertise.
We need lots of ‘tall poppies’ in the NHS, peer leaders and partners in true strategic coproduction, who are able to contribute their expertise. It’s important to recognise peer leaders will have particular expertise and may work at different levels of the NHS, from local to national, from service provision level to overall strategic, directorial and management level, from roles needing specific experience on a certain topic to peer leaders working across-the-board on various subjects. We need people who are prepared to stand out, to speak up, and to be role models to others. We need to lead by example. We need to value the contributions patients and carers and the public can bring, their unique voices, their personal power, and their expertise and experience. We need to remove this feeling of being an imposter when you start out as a peer leader, or when you join a new board or take up a new role. We need to make patients equal partners in every level of the system. We also need professionals to be ‘tall poppies’ and to advocate for the involvement of peer leaders/people with lived experience, who will lead by example by utilising and enabling true coproduction, who will role model to other professionals and leaders in the system, and who will stick their head above the parapet to ensure strategic coproduction becomes the norm.
I no longer feel like an imposter and recognise my own power and expertise. I also feel like I am a ‘tall poppy’ who is role modelling, effecting change, advocating, empowering and leading the way in the roles I hold and the boards I sit on to show the true value and vitality of strategic coproduction and the involvement of people with lived experience. I am weathering the challenges, being persistent, and sticking my head above the parapet to make sure change happens. Will you be a ‘tall poppy’, too?





Humbling, thought-provoking and timely – thank you.