What if we viewed lived experience as an asset? As an asset of professional, economic,…
Christmas in Italy Concert in aid of The Wingate Institute – My Speech
I was asked to speak at the Chelsea Chamber Choir’s Christmas in Italy concert, the beneficiary being The Wingate Institute, a prestigious, world-renowned research institute dedicated to neurogastroenterology, particularly gut failure. I was asked to speak by my consultant Professor Qasim Aziz, who has been treating me for over 5 years now, as he is Director of The Wingate Institute.
Here is my speech, and what an honour it is to have spoken there.
My name is Lucy Watts and I am 22 years old. I am speaking here today about my journey with my conditions and why the research performed by The Wingate Institute is so vital to me and so many other patients like me, in the UK and all over the world.
I became ill when I was 14 after a childhood full of problems that were never connected. It wasn’t until I started using a wheelchair that I was diagnosed with a condition called Ehlers-Danlos Syndrome in which faulty collagen results in the tissues of my body being fragile and stretchy. However by March 2009 I couldn’t eat, I couldn’t swallow very well, I suffered intense abdominal pain and bloating and my gut didn’t move at all, causing severe constipation and vomiting. I lost 6 stones in 6 months between February to August 2009. By August, I was severely malnourished and dehydrated from not being able to eat or drink and so I had an NG tube placed into my stomach, and feed pumped through this, bypassing the swallowing process.
3 months later a more permanent tube was placed directly through my abdomen into my stomach. The weight loss continued and my gut struggled to tolerate these feeds. Baffled by my case, and some professionals disbelieving that my gut problems were real, I was referred to Professor Qasim Aziz at The Royal London. I first saw Prof in April 2010; finally someone listened to me, understood what was going on, organised the right tests and we worked together to improve the function of my digestive system. I had a multitude of tests in 2010 to try and find the cause of the gut problems and as a result I was diagnosed with Chronic Intestinal Pseudo Obstruction. A full thickness bowel biopsy in 2012 confirmed this. Chronic Intestinal Pseudo Obstruction is a condition of the digestive system, in which the nerves and/or muscles of the gut don’t work properly or have wasted away. This means food, fluid and air do not move through the gut properly, causing a multitude of symptoms. It can also affect the bladder.
Prof Aziz and I worked our way through the available treatments, trying to get my gut moving. We tried everything possible, to no avail. We moved onto feeding directly into my small bowel, bypassing my stomach, however this also failed. In May 2011, weighing under 7 stones, which is dangerously low for someone of 6 ft 1, I was admitted to The Royal London by Professor Aziz and his colleague Dr Glynn. I was started on TPN, or Total Parenteral Nutrition, which is feeding directly into the bloodstream. It completely bypasses the digestive system. This comes with huge risks such as infections in the lines it’s delivered through, and liver failure. However without it, I wouldn’t survive. I’m lucky I tolerated the feed after so long without nutrition. My mum was trained to put up the TPN and to access my line using aseptic technique, and then I came home 5 weeks later. TPN continues to keep me alive.
The medications we tried all failed, despite me taking 5 times the recommended dose of one drug. My gut wasn’t moving at all. Tests showed my colon was so dilated and full that one day, my bowel could tear open. So in February 2012 I had an Ileostomy formed, whereby the small bowel is brought out onto the surface of the abdomen to form a stoma, and a bag is worn over this to collect waste.
My Ileostomy didn’t stop my gut problems, and the first year after my Ileostomy was a rocky one. It was then we realised just how badly the whole of my digestive system was affected. I was not absorbing my medications, so these were switched to other forms, some of them going into the line in my chest. I was in and out of hospital with my gut completely shutting down causing excruciating pain and endless vomiting, but these lessened in frequency after my stoma was reformed as the bowel behind it had narrowed. I have been through a lot since. In 2010 I started self catheterising to empty my bladder, then had a permanent catheter placed in 2013, and then had a Urostomy formed in October 2014, whereby a piece of bowel is used to bypass the bladder, going from the kidneys out onto the surface of the abdomen where a bag collects the urine.
My conditions and needs are very complex, requiring a lot of thinking outside the box. I have been through a lot, including many, many pseudo-obstructions, almost continuous infections including infections causing me to lose my Hickman line that my TPN and medications are delivered through, being diagnosed with a number of other secondary conditions and my general condition worsening rapidly. However I have always been able to rely on Prof to find new ways of helping me. With Prof I feel part of a team, rather than just he my doctor and I the patient. We work together to improve my quality of life and to stay on top of things, and this is very valuable to me.
I have been ill almost 8 years now, and it’s been a horrendous 8 years health wise, but I have grown as a person in ways I never would have had I not been ill, had a lot of wonderful experiences through my charity work, met so many amazing people and made some wonderful friends. I’d give my illness up in a heartbeat, but I would truly miss the person I’ve become and the things I’ve done as a result of my illness. I am more than just my conditions, but they play a huge part in who I am as a person, and I am very grateful to my team for seeing me as a person first, not just a list of diagnosis’.
Please donate generously so that research can be carried out into the causes and treatments of gut failure quickly so that I and many other patients like me can enjoy the simple pleasures of life.
To learn more about The Wingate Institute, go to the Neurogastroenterology Group’s website here.
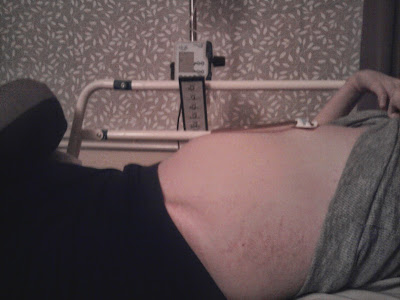 |
| Severe bloating |











This Post Has 0 Comments