What if we viewed lived experience as an asset? As an asset of professional, economic,…

Charlie Gard: A Case With No Winners
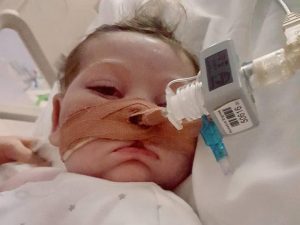
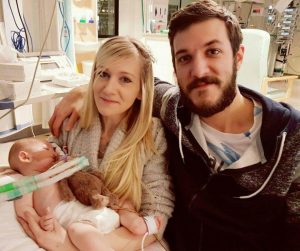
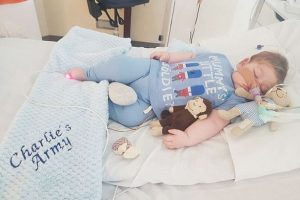
Charlie Gard. A little boy whose care has polarised the world. A little boy with a severe condition called infantile encephalomyopathic Mitochondrial DNA Depletion Syndrome. He sadly passed away last week. His doctors for months had wanted to remove his ventilation and allow him to “die with dignity”. Conversely, his parents wanted to take Charlie to America for one last chance at saving his life with an experimental treatment which hadn’t been used in his form of Mitochondrial DNA Depletion before. I can understand both sides of the story; life is precious and we all want to think we’ve done everything for our loved ones to give them a chance, even when the odds are stacked against them. Charlie’s devoted parents, Chris and Connie had raised £1.3million to take him to the US to exhaust the final chance of saving Charlie’s life. Great Ormond Street Hospital (GOSH) did not believe the medication would have had a chance of working and that it would have prolonged his suffering, that he shouldn’t be taken abroad for the treatment and his ventilation should be stopped to allow him to pass away, in receipt of palliative care to keep him comfortable.
After a long-fought battle in the courts, between Charlie’s devoted parents and with Great Ormond Street Hospital, Chris and Connie accepted that the treatment would no longer work and agreed to let Charlie pass away, but sadly their wish to move Charlie home to spend some time with him before letting him go could not be fulfilled. They were outraged, but in some cases with such complex and high-level needs, children cannot always be moved home to pass away. In the end, Charlie was moved to a hospice and had a compassionate extubation (where his ventilator was switched off and the breathing tube removed) and was allowed to pass away, aged 11 months old, just a week before his 1st birthday. I have the utmost respect for Chris and Connie for their valiant fight for Charlie’s right to life, and to one last chance at saving his life and gaining some quality of life, no matter how slim those chances were. I also applaud Great Ormond Street Hospital and their staff for their courage to care for Charlie despite the deplorable actions of the public in relation to this case which included being harassed in the street, targeted and even death threats, which is completely unacceptable. The teams were doing their utmost for Charlie, ensuring he was comfortable, pain-free and that Chris and Connie could spend quality time with Charlie, no matter the outcome of the legal case. I do not believe it should’ve gone to the courts, but I understand why it did when Charlie’s parents could not reach an agreement with the teams at Great Ormond Street Hospital, a sad situation in which there never would be any ‘winner’.
Every person has the right to life, including those of us with especially complex and life-limiting conditions. To take the position that Charlie’s condition inherently precluded him from any quality of life is incorrect. That said, Charlie’s tests did indicate that he was severely brain damaged and the team caring for Charlie and experts they brought in had the view that tests showed that, even if the treatment was to be successful, the brain damage could not be reversed.
There’s no right answer in this case, no winner and the case has polarised the world and tested ethics to the limit. I wanted to share my story in relation to the Charlie Gard case to demonstrate some of the key points featured in Charlie’s short, but poignant life.
I have followed the Charlie Gard case like many others through the press and the Charlie Gard #CharliesFight Facebook page. It has truly tested my own thoughts on life and death, because I saw the case for both sides of the argument. The right to life and parental rights, to the argument about quality of life and dying with dignity. It has made me think about my own situation and rethink things, in a way. I have felt torn about Charlie’s situation, because both sides feature arguments that are felt within my own condition and my own life.
I am a 23 year old young adult with a life-limiting condition. I’ve been in receipt of palliative care for six years. I’m kept alive by the nutritional equivalent of life support, Total Parenteral Nutrition (TPN), which provides all my nutrition and fluid via a Hickman Line into my heart, because my gut cannot digest or absorb nutrition or fluid properly. Like Charlie couldn’t survive without ventilation, I wouldn’t survive without TPN. TPN, whilst sustaining my life, comes with life-threatening complications including infections in the central lines through which the nutrition is administered into the heart, leading to bloodstream infections and sepsis (also called septicaemia), as well as blood clots and liver problems, amongst other complications. Also, the central lines required to deliver the TPN do not last forever – I myself have had eight lines in six years – and the lines do damage veins, meaning that over time access for lines can become problematic – and without central access, we can’t have the TPN and thus we won’t survive. TPN has kept me alive for over six years. It is the reason I am here today. I’m also dependent upon a tube draining my stomach, an Ileostomy and Urostomy. I undergo painful procedures and operations, including just last week to insert the third new Hickman Line in as many months. I suffer a tremendous amount as a result of my conditions and complications – I may even have a form of Mitochondrial Disease, albeit very different to Charlie’s – and as a result of the interventions I require to manage them. Pain is a part of my life, I require opioid painkillers (Fentanyl), I’m hooked up to intravenous drips at least 21 hours every day, I suffer pain from the tube in my stomach which is infected, the Urostomy that bypasses my bladder has meant that the e.coli infection in my kidneys has flourished leading to kidney problems, my digestive system is constantly painful where it cannot get rid of the acid and bile it produces and I’m wheelchair dependent, forced to spend most of my time in bed and cared for at home by intensive care nurses. However, to me, my life is still worth living, despite all I go through. My condition is progressive and will shorten my lifespan and my quality of life restricted, but to me, I’m content with the life I have. There will come a time, however, where I have to sign that Do Not Attempt CardioPulmonary Resuscitation (DNACPR) form, which I’m having to contemplate, and there may come a time where we end up withdrawing TPN and allowing nature to take its course. We also have had to put things in place including my Preferred Priorities of Care (PPC) and my Lasting Power of Attorney (LPA). I have to face the fact that my life is finite and I have had to value quality of life over quantity of life.
I’ve known I was life-limited since I was 17. I’ve had to do my end of life planning, which I am currently updating. 6 years ago when I first did my end of life planning, I didn’t make any advanced directive or sign a Do Not Attempt CardioPulmonary Resuscitation (DNACPR, also called a DNR of DNAR), just ensured my wishes for where I want to be cared for in life and also at the end of my life were documented. I felt strongly in 2011 that I wanted to be resuscitated. I felt very much that I wanted to live for as long as possible, almost at any cost. In the 6 years since then an awful lot has happened and an awful lot has changed. 6 years ago doing that end of life planning, I didn’t feel like I was life-limited. I was certain I’d far exceed any prognosis. I’d be the one to defied the odds. That I would live beyond young adulthood, into middle age, or even beyond. In my mind’s eye, I didn’t see my life being short. As such, talking about my wishes back then was easy, especially as we only did my Preferred Priorities of Care and Preferred Place of Death, not any advance decisions or refusals of treatments or interventions. In the last year, there’s been an enormous change in my condition. The decline is evident. I feel like I’m on a slippery slope, I can see the decline in my conditions, my abilities, my energy and my pain and other symptoms. I can feel that my life will be cut short, my my mind’s eye acknowledges that time is not something I will have in abundance and I won’t live a long life and far exceed the prognoses I may be given. I was told I’d be lucky to get 5 years in 2012; I’m fortunate to have made it to this point. My hospice nurse and I have had some frank conversations, I know I need to get everything in order. I hope I have a life ahead of me for now, that I will keep going for as long as possible, but I have to prepare for my death. I also have had to accept the likelihood that my death will not be a slow and gradual process where I have time to prepare and slowly drift out of the world, I’ve been told that it’s likely an infection causing sepsis that’ll claim my life and that will be sudden. I have to prepare now, whilst I still can, for the occasion when my life will end. I’m having to do a lot of soul searching, talking to myself and asking what my true wishes are. I don’t want to die, I’m terrified of dying because I don’t want the amazing life I have now to end. However, I cannot live in denial. I have to face the fact that resuscitating me is probably a futile prolongation of suffering. My body, if it did survive a cardiac arrest, would likely come out the other side with a restricted quality of life and severe problems and repercussions. Do I want to live without quality of life? No. The answer is no. I want to live my life so long as I have quality of life – I’ve always been of the opinion of quality over quantity.
The conversations I’ve had with my hospice nurse and my deep thinking, usually at night (as it is in writing this), has truly made me reconsider what I really want and what decisions I need to make about my treatments and care. I really should sign a DNACPR, purely as efforts would almost certainly be futile and if successful, the chances of having any quality of life if I survived is slim. However, I just don’t feel able to sign that paperwork. It feels like I’m giving up on myself. I need to truly think about my chances, what my wishes are, what I define as quality of life and whether I would want suffering to be prolonged when I would have no quality of life? I need to seriously consider and face up to the DNACPR and/or an Advanced Directive. For example, my lungs are weakening. If I were to be intubated, it’s not likely I would be able to be extubated. I need to make these decisions for myself and not leave my family with horrendous, heart wrenching decisions if I were unable to make decisions for myself. I am in the process of doing my Lasting Power of Attorney too, so that my mum can make decisions of my behalf if I lacked capacity. I’ve had accept a lot of painful truths and think about what is in my best interests, what is acceptable in terms of quality of life and make decisions to ensure my suffering isn’t needlessly prolonged, that my wishes are respected and my family are not left with difficult decisions that they cannot consult me about. I need to accept the truth and to make every preparation I can.
The difference between myself and Charlie is that I am an adult and I can speak for myself and make preparations for future care. I can express my pain or my wishes. I can make decisions about my life. Charlie couldn’t. Charlie’s parents had to fight for what they felt was right for their son; a chance at life, no matter how slim the odds. I also understand the perspective of the medical professionals looking after Charlie at the world-renowned Great Ormond Street Hospital (GOSH). They felt, in Charlie’s best interests, it was kindest to turn off the life support on which he depended, as they feel he was suffering and that there was no meaningful chance of any improvement in his condition. Who is right? I for one don’t know.
I have been appalled at the hate and negativity directed at Great Ormond Street Hospital, however. I understand the feelings on both sides of the ‘debate’ over what the right answer was in Charlie’s case. However, I also know for some, standing back and being objective when it’s so difficult, emotional and it’s your loved one who you’re being told should be allowed to pass away, is almost impossible. You’re too emotionally invested. It’s just a shame that a decision couldn’t be reached between Charlie’s family and the teams at Great Ormond Street and that it had to go to the courts. I understand the wish for Charlie to have one last chance at life, I think about myself and how I’d feel if I was told that my TPN would be withdrawn – a death sentence – and how my mum and sister and extended family would feel in that situation. Could they be objective? I am not sure. However, the difference is, my mum and I have had long conversations and she knows my wishes intimately and what I would and wouldn’t want. Charlie couldn’t communicate whether he was suffering or what he’d want to happen. All his family could go on was what they felt were in his best interests. All Great Ormond Street could go on was the scans and test results and the fact that the treatment had never been used in Charlie’s condition as well as the fact he had brain damage that they felt couldn’t be reversed, therefore they believed it was in Charlie’s best interests to extubate him and allow him to pass away naturally. What was in Charlie’s best interests? We will never have a concrete answer to that, as it relied on the opinions of those close to and involved in Charlie’s life and his care. Since an agreeable decision couldn’t be reached, it was one opinion versus another. We will never know what the right answer was. I do believe that the parents’ right to decide the treatment of their child is important and considering they’d raised the money to take him to America for treatment, the feeling of “why couldn’t they have one last chance?”. I also understand that Charlie was possibly suffering and that the kindest thing to do would be to let him go. I felt very torn by his case.
One of my friends lost her daughter at Great Ormond Street in the same ITU after having to make a similar decision to Chris and Connie. She had to make the decision to turn off D’s life support. D had a life-limiting condition and had been supported by the hospice since she was 6 months old and by the palliative care team since she was 7. Her family had been forced to prepare, make decisions and accept that D’s life would be short. In the end, D’s mum desperately wanted to get her home to pass away, after she developed septic shock and there was no way she could ever overcome it. The requirement for this to be possible would be to extubate her, put her in an ambulance and get her home – but the likelihood would be that D would die in the ambulance on the way home. The same with the hospice. It just wasn’t an option. D’s mum decided to turn off her life support, surrounded by her mum and siblings, in the ITU. D’s mum said that, at the end, all that mattered was that D knew she was loved and was surrounded by her beloved family. They were together as the life support was switched off and D passed away. It was a tough decision for D’s mum to make, but at the end of the day, it wasn’t the location that mattered but that D was surrounded by the people she loved. She wrote a blog about this and I wanted to share the link with you, as I feel it is compulsory reading for those on both sides of the Charlie Gard case debate. Click here to read it.
My message at the end of this that in cases like these, there’s no winners. The treatment of Great Ormond Street and its staff was not acceptable. I understand it is a very emotive situation and we all wanted what was best for little Charlie, but that does not excuse the behaviour that occurred. The most important thing in all of this was Charlie and his family.
It’s easy to imagine what we’d do in a certain situation, but it’s different if you truly live it. I can only imagine the pain and heartache Chris, Connie and family have gone through and are continuing to suffer following the loss of their beautiful, precious little Charlie. My thoughts are with them. However my thoughts are also with the healthcare professionals who have looked after Charlie who’ve had much negative press. I extend my gratitude as a human being to those professionals for the care they provided Charlie; they, too, will feel the loss of Charlie as they do every patient they lose.
Sleep tight Charlie. May you rest peacefully and watch over your mummy and daddy. They love you very much.
Charlie Gard photos (c) of Chris Gard and Connie Yates.






This is such a beautifully written and thoughtful post Lucy. Despite having a number of chronic conditions, I can't even imagine what it must feel like to have to make the decisions that you are having to face. But you speak about these choices so eloquently. And your take on Charlie's case comes from real understanding of both 'sides' of the coin. I think this will really help people to understand what an awful situation something like this is for both family and medical professionals. Like you say, there is never going to be a winner in cases like this. Take care lovely.
Jenny xx
http://www.jaffacat.co.uk