What if we viewed lived experience as an asset? As an asset of professional, economic,…

Accessibility, Complex Needs & Hospitals – A Blog In Honour of Adam Bojelian
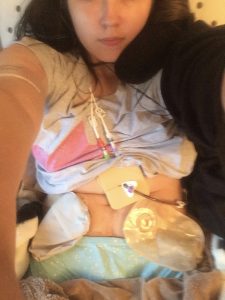
I’m a 24 year old young lady with a life-limiting condition that has caused complex physical and medical needs. I am completely dependent on a specialist electric wheelchair, although forced to spend a lot of time in bed, I require the use of a hoist to be moved, I need help with all activities of daily living as I require two people to attend to all of my personal needs and I have multiple organ failure which means I am dependent upon feeding directly into my bloodstream (TPN) via a central line into my heart, I receive my medication through this line also, as well as having a tube constantly draining my stomach and two stoma bags; an Ileostomy, where the end of the small bowel is brought out onto the surface of my abdomen over which I wear a bag to collect bodily waste and a Urostomy, where a piece of bowel is cut free from the digestive tract and is used to form a tube between the kidneys and ureters onto the surface of my abdomen and I wear a bag over this to collect my urine. I have been in receipt of palliative care since I was 17 years old and in fact, was not expected to reach my 24th birthday. I require 24 hour care. At home I have a care package consisting of one-to-one care from an intensive care nurse for a minimum of 16 hours a day, I have an overnight carer to attend to my needs at night and then I also require a second person during the day to support the nurse to attend to my physical, mobility and personal care needs. This is funded by the NHS via Continuing Healthcare (CHC) as my needs are purely health needs, albeit it means that my social needs are neglected.
I spend a lot of time in hospital. My condition means that I am cared for at multiple hospitals under a variety of consultants from various specialties, as well as being supported by other healthcare professionals such as a palliative care nurse, occupational therapist, district (community) nurses, physiotherapist and clinical nurse specialists for nutrition and central lines, and stoma care. I suffer frequent bouts of sepsis (formally known as septicaemia), which is a systemic bloodstream infection causing my immune system to overreact, causing organ dysfunction and even damage and other complications. I’ve suffered sepsis 12 times; I am lucky to be alive. I have four chronic, incurable, multi-resistant infections in my body, all of which have the potential to make me seriously ill with sepsis at any time. We have been told that, although my condition is life-limiting, it is likely an infection causing sepsis that will end my life. I’ve spent so much time in hospital fighting for my life with sepsis, I’ve had admissions for treatments, I’ve had admissions for operations, I’ve had admissions for complications of my conditions and I’ve had admissions due to problems with my central line. I’ve spent an awful lot of time in hospital, but we are able to try and manage things at home as best we can, whenever and for as long as possible.
I face battles with accessibility in my daily life. I face battles to get the care I need. I’ve spend my life fighting for support and to be able to access the things I want and need to. Would you believe it if I said hospitals are some of the worst places for accessibility? Would you believe that they are often some of the most difficult environments for people like me with complex disabilities? Well, I am going to explain why hospital admissions are such a challenging, inaccessible environment for people like myself.
I require one-to-one, 24 hour care. I have very intensive needs, some of which require training above the typical nurses’ training. My needs take up a lot of time to attend to and often require two people at one time. What ward nurses, in today’s climate, can spend more than 8 hours caring solely, intensely for one patient? What wards can spare one nurse and one healthcare assistant to spend up to two hours washing and changing a single patient? When I go into hospital, if my mother does not stay with me and undertake all of my care – intravenous feeding (TPN) and fluids and intravenous drugs included – I end up going without 70% of my needs met as ward staff do not have the time to devote solely to me. This means, at a time when I am poorly enough to be in hospital, I am forced to go without some of the things I need when well – let alone needing them when poorly! Fortunately I have my mum to stay with me, as my homecare package is stopped by the CCG upon admission to hospital, meaning the 24 hour care I receive at home is gone. The simple solution would be to place me in the high dependency unit, where I can receive more intensive care from suitably trained nurses, but no hospital will give up an HDU bed for someone who isn’t seriously ill enough to warrant taking up that bed. Mum has to stay, or leave me at risk.
However, it’s not just the actual care itself that is the issue. Hospitals aren’t geared up for people with complex disabilities. They aren’t geared to our needs. Often the hospital bathrooms aren’t big enough for a wheelchair and two people, let alone a wheelchair, two people and a hoist. Fortunately, I do not ever need to transfer onto the toilet anymore as I have two stoma bags, but when I did, I was forced to use a commode beside the bed because you couldn’t fit myself, my wheelchair and two people in to assist me to transfer onto the toilet. I had to give up my dignity over a lack of accessibility.
Then there’s showering. No hospital wards have an accessible bath – or if some do, I’ve never encountered one – nor a changing table or shower bed to shower people who need to be laid down. This means we’re reduced to bed baths – once again, we lose dignity – over a lack of accessibility.
Hospital rooms aren’t always set up to accommodate big wheelchairs let alone bays. It means we’re squeezing everything in to try and get me in and out of bed – bays and side-rooms aren’t set up to accommodate a bed, a hoist and a wheelchair as well as at least 3 people (two to hoist, one to manage my drips and bags).
Hospital bed-sides often don’t have enough plug sockets. This means my bed, mattress, pumps and wheelchair charger can’t always be plugged in all at once. Let alone for me to be able to plug in my own things, like my phone, my laptop and anything else. We end up bringing in extension leads, which are checked by the hospital, just so that we can fit all of our electrical items – especially all my medical electrical items – in beside my bed. Some bedsides only have 2 plug sockets – that would only allow me to plug in 2 vital electrical items – I have 5 medical items alone that need to be plugged in at any one time.
Due to my needs, I frequently am not able to get out of bed in hospital at all. Due to the amount of people it takes, my complexity of needs, the space and the lack of staff means I can be completely stuck in bed for over a month whilst in hospital. I’m being prevented from leaving my bed due to my disabilities and the complexity and intensity of my needs. Another thing I struggle with in hospital, is the lack of wifi and poor signal. This means I am completely isolated from the outside world – I can’t even go out of the ward – and being in London means I am away from family and friends, so I can be completely cut off from the world for the duration of my admission.
Sadly, I’ve had some bad experiences that are brought about purely due to a lack of accessibility in hospital. I have repeatedly been manhandled out of my wheelchair and onto a hospital bed or trolley due to a lack of hoists or hoists being broken or incompatibility of my home sling to hospital hoists – for which I have since had to spend a sum of my own money to purchase adapters to make my sling compatible (I can’t use their slings as I have a custom sling and once sat in my sling, you can’t take it out or get a new one underneath me). I’ve been manhandled out of my wheelchair and into a bed or onto a trolley multiple times, which has caused great pain. One such incident was this. I turned up for a procedure having informed them that I would need to be hoisted onto the trolley as I could not transfer. The agreement was I would go onto the medical day-stay unit to be hoisted out of my wheelchair and onto the trolley where I would then be wheeled through to interventional radiology to wait for and have my procedure. We turned up at the day unit and they refused to hoist me into the trolley, insisting IR have a hoist (which I knew they didn’t and informed them of this). We were on the day stay unit for over an hour and every time we asked about them hoisting me onto a trolley we were told IR had a hoist and would hoist me themselves. Eventually it was time for me to go into IR and I was taken through in my wheelchair. IR then asked me to get onto the bed, so I explained I needed to be hoisted and that was why I was on the day stay unit, and explained day stay had told us IR had a hoist. IR don’t have a hoist, as we already knew. The next thing, the team in IR are trying to convince me that if I try hard enough, with their help I could transfer onto the trolley. I repeatedly explained I cannot weight-bear at all so I cannot transfer even with support. Then the team were frustrated. I explained the whole situation and they then said to the day stay unit could they use their hoist in IR to transfer me, only to be told the hoist can’t be taken out of the day unit and that now I was an IR patient, I could not go back into the day stay unit to be hoisted and they didn’t have time anyway. Also, they informed us they didn’t even know where the hoist was. As such, the IR team, using my sling, manhandled me out of my wheelchair and onto the bed, causing me great pain and leaving me with bruises and discomfort from scraping over things and being dragged out of my wheelchair and onto the trolley. However, we got me onto the trolley ready for my Hickman Line change. Worse was still to come, though, when I came out after the procedure. It had been an extremely traumatic and painful insertion (I have them done awake with local anaesthetic) and I was very bruised, sore and quite upset at how traumatic it had been. 15 minutes after my Hickman Line insertion, after which you’re supposed to be careful movement wise so not to dislodge it, I was manhandled back off the trolley and into my wheelchair. It reduced me to floods of tears, the pain was absolutely excruciating. It was a very traumatic and upsetting and painful day. This is not an isolated incident, though. I needed X-rays done at a hospital and had explained at length with the department that they needed a hoist available to get me onto the table and was assured the hoist had been booked, organised and would be there to hoist me. Except, when I arrived, there was no hoist. There was no hoist anywhere to be found. Once again, I had to be manhandled out of my wheelchair using my sling and onto the X-ray table, spend 45 minutes being X-rayed, in a lot of pain, then to be manhandled back off the table and into my wheelchair. These departments knew in advance I needed to be hoisted and for a hoist to be available, and yet there was no hoist and so I was painfully manhandled from wheelchair to bed and vice versa because people had not listened or organised hoists despite plenty of prior warning and double checking. These aren’t isolated incidents at all. It’s actually quite commonplace for me.
A few years ago, I was able to transfer with a lot of help. I could just about put weight through my legs but only for a very short few seconds, so transferring was a case of people getting me to my feet and guiding me to turn and get me down onto the desired place before I fell to the floor. It wasn’t exactly safe, but I fought for so long not to be hoisted knowing how difficult it would make things. However, late 2015 it started to become increasingly more difficult but above all, dangerous. Having got osteoporosis and already having broken my hip requiring a dynamic hip screw and plate aged 20, I couldn’t risk falling. Not only that, but my muscles were just too weak to do it anymore. I stopped being able to weight-bear in March 2016 and got my first hoist a few months later. Since getting the hoist, I’ve only managed 1 supported transfer that didn’t go as planned, so we know it is just not possible anymore. At 6ft 1 tall and 82kg, there is no way I can be lifted or carried, so hoisting is my only way to be able to transfer.
Of all places, people think a hospital, which is designed for sick people, would be completely accessible and cater to the needs of all patients, from mobile and self-caring down to completely dependent people with complex needs, like myself. Sadly, hospitals are not catered to people like me. They don’t have the facilities, equipment, staff, ward and room design for people like myself. Not only that, but the lack of staff, let alone the lack of staff trained in specialist procedures, and an increasing number of patients per nurse greatly impacts upon our care. As such, my needs often go unmet in hospital. Without our parents, we would go without basic and vital needs met. That is, unless the patient’s home-care package can continue whilst they’re in hospital, so the home staff can provide one-to-one care whilst in hospital, to allow the patient’s needs to be met fully. This is sadly not allowed in my case. If my mum didn’t stay, many of my basic and some vital needs would go unmet, due to lack of staffing, lack of trained staff and the sheer amount of time it takes to attend to my needs alone. Hospital stays without Mum reduces me to prioritising my needs and hoping I can get the most important ones done at the expense of the less pressing needs, such as going without a wash in order that all my IVs can be done and my stoma bags can be changed, the latter of which can take an hour and a half or more. With Mum, 100% of my needs will be met.
As you can see, I’m a young adult with complex medical needs who struggles with the inaccessibility of hospitals and the limited ability of hospital staff to fully meet the needs of people like me with complex, specialist, intensive and time-consuming care needs.
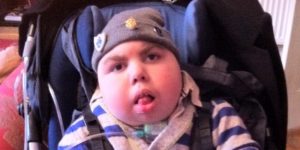
I’ve written this blog in honour of #AdsLegacy at the suggestion of his wonderful mother Zoe. If you haven’t heard of Ads, full name Adam Alexander Bojelian, you’ve certainly missed out. Adam was a writer, poet, campaigner and inspiring patient leader whose only method of communication was using his eyes; he could not talk, meaning blinking was his voice. As Adam could not speak, this led people outside his family, such as professionals, to write him off as non-cognitive, but inside Adam was this incredible mind, a mind unlimited unlike the limits of his body, with a breathtaking talent for words and for poetry; a mind like no other. He’d blink to the correct letters or words, painstakingly constructing his poetry, blogs or other pieces. He received a Brit Award for writing, no less, and was a fellow HSJ Top 50 Patient Leader in 2015; it is a privilege to have been on that top 50 list with him. Did I mention Ads achieved this all by the age of just 15, when he sadly died as a result of sepsis? Now if you don’t think that’s incredible, there’s something wrong with you. Adam would be 18 this coming year and his family, supported by all of us friends and followers, will be undertaking a campaign to improve the care in hospital of children and young people – and adults – with complex needs, to ensure the equipment we require is available, wards and rooms and clinics are accessible, our needs are met, staff understand how to support us and that our dignity and our rights will be upheld. If you didn’t know Adam, you do now. Follow @4AdsThePoet on Twitter to learn about and celebrate his legacy and go to his blog here. Also, consider joining us for the #Ads2018 talk in Leeds in March, to celebrate his life and work together to create change.
Thank you.






After reading this I do not feel sorry for you because braver and stronger than all of us. Thank you for sharing your story and inspiring me. Hope all your struggles end soon.